Delivery skills save the life of mother and baby
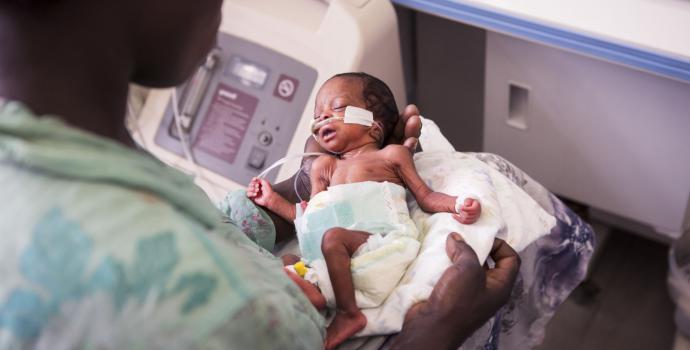
At the end of May a first-time mother arrived at Rwebisengo Health Centre III in the early stages of labour and in critical condition.
She needed emergency attention to save her baby.
Ainembabazi Brenda was on duty. She is the only midwife attached to this rural health centre in Ntoroko district, western Uganda. With support from a comprehensive nurse and sometimes volunteer midwives, Brenda is in charge of maternal and newborn health services.
She quickly identified a case of “cord prolapse”, a labour complication where the umbilical cord of the baby presents before the baby’s head.
“Cord prolapse presents a great danger to the baby," says Brenda, "since there can be a cut off of oxygen supply to the baby if this is not handled skillfully and immediately.”
In such a setting the mother is supposed to be quickly referred to a health centre with Comprehensive Emergency Obstetric Newborn Care services, where a C-section can be performed to save the baby.
But in remote rural areas that cannot always be done quickly. At Rwebisengo there is no motor vehicle ambulance, so the main means of transport for referral is a motorcycle ambulance or on the back of a commercial motorcycle. There is a bigger health centre at Karugutu 38 kms away and a regional hospital at Fort Portal 70 kms away, but a motorcycle journey to either referral centre can be slow and dangerous in such a critical condition. An ambulance can be sent from Karugutu but can take too time in an emergency and may require the patient’s family to contribute funds for fuel.
“Given the challenges with emergency transportation, referral would be risky,” says Brenda.
Brenda has worked at the health centre for three years and received various training and mentorship from Save the Children to enhance her skills on maternal and newborn care. “I’ve received training in Helping Babies Breathe, delivery skills, Focused Antenatal Care, eMTCT (Elimination of Mother-to-child transmission) and Community Newborn Care, among others,” she says.
According to Brenda, this training proved life-saving.
“With the skills attained in the delivery care training and mentorships, I put the mother in the knee-chest position to relieve the pressure on the cord,” she explains.
“An I.V line was also put to keep the mother hydrated and to provide enough energy supply to the baby to limit distress. I monitored the fetal heart of the baby and labour progressed. Guiding the cord and elevating the head a little higher the mother was able to deliver a live baby within an hour after arriving at the health facility. The baby scored 10/10 APGAR (a quick test performed on a baby a few minutes after birth) which medically indicated that the newborn’s health status was normal.”
“I believe my delivery skills enhanced through the Save the Children training gave me the confidence to handle this case since there was limited time and means to support referral, which could have put the baby at a higher risk. The mother and the baby were monitored for the next four days and were discharged in good condition.”
The Health System Strengthening programme in western Uganda is supported by Save the Children Korea





