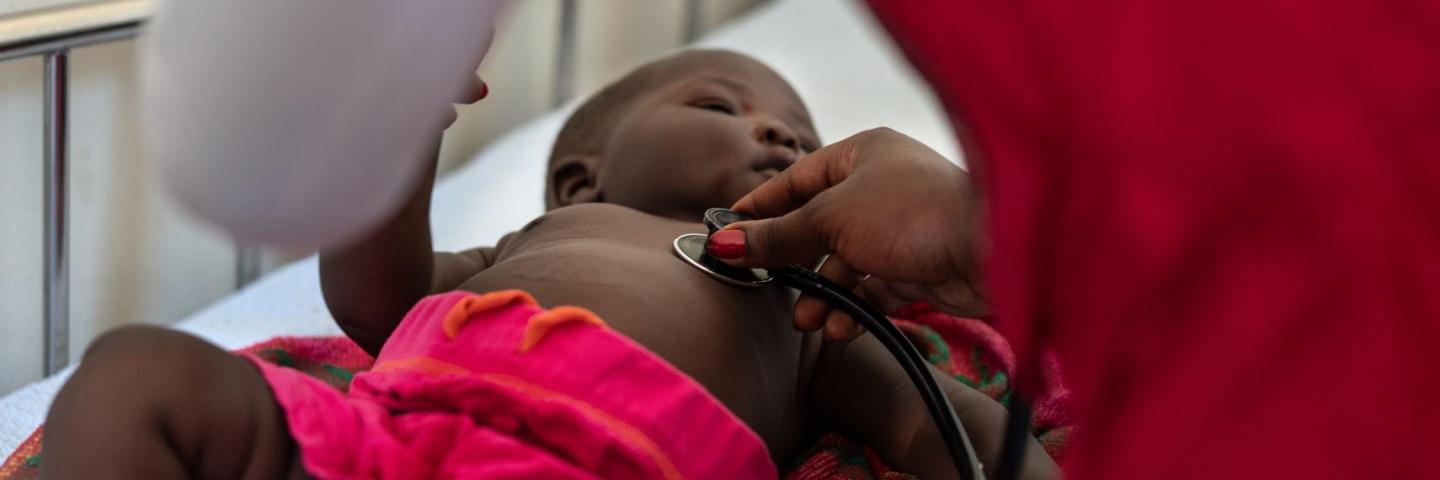
The last two decades have brought some important improvements in health indicators in Uganda. Maternal and under-5 mortality have decreased by around 50 percent, thanks to widespread immunisation campaigns, increased antenatal care and better access to health facilities. However, these rates remain very high and most children still do not have adequate healthcare. Health facilities are often in dilapidated condition and run out of drugs and electricity. Services for babies born prematurely or with complications are often not available. 29 percent of Ugandan children under five years old suffer from chronic malnutrition, known as stunting, which prevents their mental and physical development. Despite some progress, millions of children are being left behind.
Improving Maternal and Newborn Child Health (MNCH)
We support district authorities to improve access to quality MNCH services and get more mothers giving birth at equipped institutions rather than at home. In remote rural communities of Uganda our approach has helped reduce neonatal mortality by 51 percent and the number of children dying before their fifth birthday by 42 percent.
We use a systems strengthening approach to train health workers on specialised care; equip clinics and hospitals with vital resources such as lifesaving resuscitation equipment, oxygen cylinders and incubators; and educate parents and pregnant women about good practices. We support local health committees and more than 1,000 Village Health Teams (VHTs) to disseminate information in the communities; and pilot innovative approaches, such as using motorbike ambulance taxis to reach pregnant women in the most inaccessible villages.
WATCH: Motorbike ambulances help Ntoroko residents grappling with poor health services
LISTEN: Podcast: The women who left everything behind
Saving Newborn Lives
The first minutes and hours of a baby's life are critical, so we promote simple steps that can save lives. We train mothers on 'Kangaroo Mother Care' where skin-to-skin contact and breastfeeding offer children warmth and nutrition at the most critical stage after birth. Asphyxia, or inability to breathe, is the biggest killer of newborn babies in Uganda, so we train nurses and midwives on basic skills to resuscitate babies immediately after birth.

Promoting Adolescent Sexual and Reproductive Health (SRH)
Adolescents in Uganda do not have adequate access to sexual and reproductive health services or information. At least one in four women in Uganda get pregnant as a teenager, contraceptive use is limited, and teenage pregnancy is a key factor in girls dropping out of school. We work with schools, clinics, youth peer groups, village health teams and other platforms to increase adolescent knowledge of sexual and reproductive health. We support youth champions to spread messages and act as change agents in their communities.
Boosting nutrition
Our Infant and Young Child Feeding (IYCF) programmes provide malnutrition screening, food and nutritional support to young children and their mothers. In the refugee settlements we run Mother & Baby Areas (MBAs) which promote breastfeeding and good nutrition among pregnant and lactating women and caregivers for children under two years old. Practising optimal IYCF, including breastfeeding and complementary feeding, is the most effective way to reduce child malnutrition in emergency settings.
READ: Isabella - a champion for breastfeeding
Responding to emergencies
We work with the government to prevent and respond to deadly outbreaks when necessary. To prevent the spread of Ebola from neighbouring DR Congo we have trained health workers, provided equipment to hospitals and clinics, and run community awareness campaigns to dispel myths and rumours and provide accurate information.
READ: Information can save lives as Ebola spreads
System strengthening
Sustainable long-term change will only be possible if basic health systems are in place and strengthened. We work to improve the capacity of health facilities, strengthen leadership and governance structures and community health committees, and engage in national policy and technical working groups. We also support research and development. For example, we supported Makerere University School of Public Health to establish the Maternal and Newborn Child Health Centre of Excellence, the first of its kind in sub-Saharan Africa.
Last year our health programmes reached 182,000 people across Uganda.